Statins are a group of medicines that help lower cholesterol levels in the blood.
They have been around since the 1980s and are widely prescribed for high cholesterol when lifestyle changes have not been enough to lower cholesterol to healthy levels.
Lowering high cholesterol is important. If left untreated, it can increase the risk of a heart attack or stroke.
This is because high cholesterol can cause the build-up of fatty material (plaques) in the walls of the arteries, causing them to narrow. This is a process called atherosclerosis.
There’s lots of research showing statins are safe and effective. Studies show they can lower your ‘bad’ LDL cholesterol by up to 30 per cent at low doses, and more than 40 per cent at the highest doses.
Most people have no side effects from statins. However, some people do, most commonly muscle pains and aches.
This means they need to take an alternative cholesterol-lowering medicine. And others may need to take another medicine, as well as a statin, to help bring their cholesterol levels down to healthy levels.
Here we look at 4 medicines that doctors can prescribe as an alternative, or add-on, to statins.
1. Ezetimibe
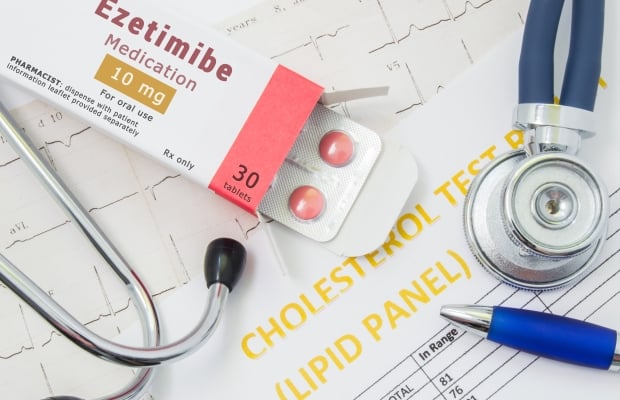
This comes as a tablet that’s taken once a day. It works by blocking the absorption of cholesterol from food in your stomach into the bloodstream, which leads to lower cholesterol levels.
This means the liver has to use more cholesterol from the blood to make bile, which is an essential substance for digestion. This, in turn, lowers blood cholesterol levels even further.
The National Institute for Health and Care Excellence (NICE) says doctors can prescribe ezetimibe for people who cannot take statins due to side effects, or alongside statins in those who need extra help to lower their cholesterol levels.
However, it’s not as effective as most statins on its own. Ezetimibe lowers ‘bad’ LDL cholesterol by 15 to 22 per cent when used alone, but when taken with a statin it lowers it by 21 to 27 per cent.
Possible side effects include stomach pain, diarrhoea, flatulence and tiredness.
2. Bempedoic acid
This cholesterol-lowering medicine only came into use in the UK in 2021. It’s taken daily and comes as its own pill or in a combined pill with ezetimibe (see below).
Like statins, bempedoic acid reduces the production of cholesterol in the liver, which in turn lowers cholesterol levels in the blood.
But it differs from statins in that it only works in the liver, so there’s less risk of side effects like muscle pain.
However, it’s not quite as effective as a statin on its own, only lowering ‘bad’ LDL cholesterol by 17 to 28 per cent. When taken with ezetimibe it’s more effective, giving around a 28 per cent reduction in cholesterol levels.
For this reason, NICE says it should only be prescribed with ezetimibe – either for people who cannot take statins due to side effects, or when ezetimibe does not lower cholesterol enough on its own.
Common side effects include a lack of red blood cells (anaemia), gout, high levels of uric acid in the blood, and pain in the hands, feet and arms.
3. PCSK9 inhibitors
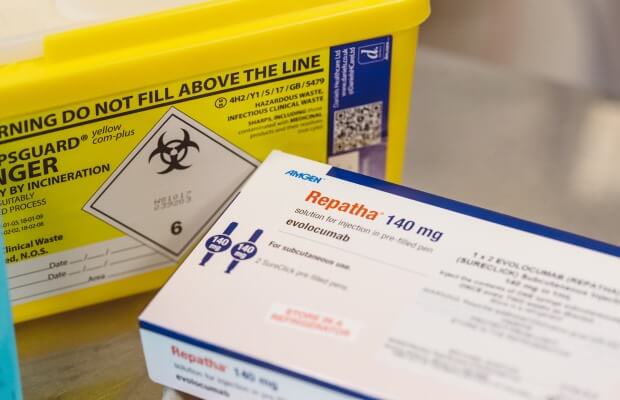
These are given as an injection under the skin every 2 to 4 weeks. They stop a protein called PCSK9 from working, which then allows the liver to remove more ‘bad’ LDL cholesterol from the blood.
Studies show that PCSK9 inhibitors can lower ‘bad’ LDL cholesterol by up to 60 per cent. In people with heart and circulatory diseases, they also reduce the risk of death from a heart condition or having a heart attack or stroke by 20 per cent.
NICE recommends PCSK9 inhibitors only for people who have had a heart attack or stroke already, where the maximum dose of statins has not lowered their cholesterol to the desired level.
People with a genetic condition called familial hypercholesterolaemia, which can lead to very high cholesterol levels, are also eligible for NHS prescriptions.
Reported side effects are few but include flu-like symptoms or soreness around the injection site.
4. Inclisiran
This is one of a new class of medicines known as gene-silencing drugs.
Inclisiran works similarly to PCSK9 inhibitors, but it uses RNA therapy to block or ‘silence’ the gene that produces the PCSK9 protein, rather than acting on the protein itself like PCSK9 inhibitors.
This boosts the liver’s ability to remove harmful cholesterol from the blood.
It is given as an injection under the skin. After an initial dose, another injection is given 3 months later, and then you only need injections twice a year after that.
Trials show that inclisiran can reduce ‘bad’ LDL cholesterol by up to 52 per cent.
However, under NICE guidance, it can only be prescribed to people who have had a heart attack or stroke, when statins have not lowered their cholesterol levels enough.
It can be given on its own, or with statins and other cholesterol-lowering drugs, except PCSK9 inhibitors.
Reported side effects include pain and redness or a rash at the injection site.
What to read next...



