Improved care for people with long-term conditions
In three years, the BHF House of Care programme has made good progress towards implementing a care and support planning approach to support people with long-term conditions.
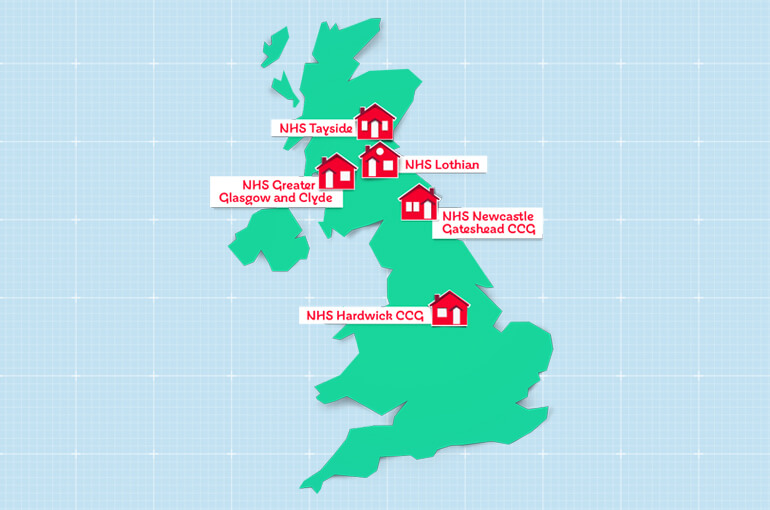
As a result of the BHF House of Care programme, care and support planning is now live in 41 practicese and 13,061 people received a review through the programme.1
Across all sites, people with LTCs reported a good level of involvement in their own care.2 Sites used evaluation toolsf to record project impact, including questionnaires at baseline (in 2016-17, as sites were establishing care and support planning) and at follow-up (in 2017-18, after care and support planning had been embedded in sites).
An analysis of questionnaire responses across sites found that between baseline and follow-up, there was an increase in people feeling their care was ‘almost always’ joined up (from 56% to 60%).3 They said appointments felt less rushed and 59% of patients said they ‘almost always’ discussed what was important for them in managing their health.4 After the care and support planning consultation, 75% said they were ‘better’ or ‘much better’ able to understand their conditions.5
The nurses are very good and they do seem to treat you as an individual, as a person.Patient
The ‘preparation’ step of the House of Care approach is a key element. Here, people can prepare for the collaborative conversation, receiving their results – fully explained – in advance along with agenda prompts that encourage reflection on what they want to discuss in their care and support planning review. In Gateshead, 94% of patients said that the preparation letter was ‘very useful’ or ‘somewhat useful’.6 Some people said this led them to do more research about aspects of their health they hadn’t considered before, such as lifestyle changes.7
It also helped healthcare professionals “shift from a ‘fixer’ to a ‘facilitator’” who helps the person maximise their own health and wellbeing through the collaborative conversation.7
Overall, patients said they were happier with the information and support they received to help them manage their care and how healthcare professionals explained things (up from 63% to 68%).8 However, the proportion of people who said they felt ‘very confident’ in managing their own health dropped from 49% to 41%.9 Sometimes, this was linked to patients being unsure of what their results meant.7
Others felt some anxiety or stress about being more involved in the conversation.7 This suggests that patients currently feel that support is in place but confidence to self-manage with this support may be an area that needs further encouragement, including during the care and support planning process.
Next: Motivating healthcare professionals
References
e 41 practices were specifically included as part of the BHF programme and the evaluation, but more practices have adopted the approach across these five sites.
f Tools included Long Term Conditions 6 (LTC-6), Consultation Quality Index (CQI), Consultation and Relational Empathy measure (CARE) and Patient Enablement Instrument (PEI), combined to make CQI for Lothian, and the Warwick Edinburgh Mental Wellbeing Scale (WEMWBS).
1 ICF Consulting Ltd, 2018. House of Care Evaluation: Final Report [PDF], page 8
2 ICF Consulting Ltd, 2018. House of Care Evaluation: Final Report, page 60
3 ICF Consulting Ltd, 2018. House of Care Evaluation: Final Report, page 60, Table 8.5
4 ICF Consulting Ltd, 2018. House of Care Evaluation: Final Report, page 70
5 ICF Consulting Ltd, 2018. House of Care Evaluation: Final Report, page 62, Table 8.8
6 ICF Consulting Ltd, 2018. House of Care Evaluation: Final Report, Annex 3, page 16
7 CF Consulting Ltd, 2018. House of Care Evaluation: Final Report, page 71
8 ICF Consulting Ltd, 2018. House of Care Evaluation: Final Report, page 61, Table 8.6
9 ICF Consulting Ltd, 2018. House of Care Evaluation: Final Report, page 61, Table 8.7

